 The current form of the Hungarian general practitioner (‘GP’) system is unsustainable, as it is still unable to perform its role as a gatekeeper. Doctors working as retirees, the irreplaceable human resources, unorganized patient pathways, increasing workload, and untapped professional capacity result in a hospital-centric health care system while outpatient and inpatient clinics are unable to perform their original function, and increasing waiting times in all sectors of the sector weaken patients’ confidence in healthcare. On the one hand, these problems raise dilemmas about the inefficient use of public money, on the other hand, the need for an organized integration of private health into the current structure. The state is also working to reduce the growing burden on GPs, however, a lack of experience often gives rise to solutions that tend to escalate the current situation. Read more… (Máté Sándor Deák – Dóra Lovas)
The current form of the Hungarian general practitioner (‘GP’) system is unsustainable, as it is still unable to perform its role as a gatekeeper. Doctors working as retirees, the irreplaceable human resources, unorganized patient pathways, increasing workload, and untapped professional capacity result in a hospital-centric health care system while outpatient and inpatient clinics are unable to perform their original function, and increasing waiting times in all sectors of the sector weaken patients’ confidence in healthcare. On the one hand, these problems raise dilemmas about the inefficient use of public money, on the other hand, the need for an organized integration of private health into the current structure. The state is also working to reduce the growing burden on GPs, however, a lack of experience often gives rise to solutions that tend to escalate the current situation. Read more… (Máté Sándor Deák – Dóra Lovas)
The current form of the Hungarian general practitioner (‘GP’) system is unsustainable, as it is still unable to perform its role as a gatekeeper. Doctors working as retirees, the irreplaceable human resources, unorganized patient pathways, increasing workload, and untapped professional capacity result in a hospital-centric health care system while outpatient and inpatient clinics are unable to perform their original function, and increasing waiting times in all sectors of the sector weaken patients’ confidence in healthcare. On the one hand, these problems raise dilemmas about the inefficient use of public money, on the other hand, the need for an organized integration of private health into the current structure. The state is also working to reduce the growing burden on GPs, however, a lack of experience often gives rise to solutions that tend to escalate the current situation.
Introduction
 The basis of continuously available health care is the general practitioner and the pediatrician, who, together with the medical on-call services, must provide the needs and requirements of the residents of the practice 24 hours a day. The territorial care system includes the care obligation of the resident of the area. When organizing care, it must be taken to ensure that care is available at well-planned times. The walls of the GP system have been collapsing for a long time, and the most obvious evidence of this has been the inadequate functioning of the central on-call system. In the case of on-call care, every minute counts, it is important that the patient has access to life-saving and prevention of serious or permanent damage to health as soon as possible.[1] One consequence of the increasing workload on primary care is increased waiting times, which, however, are most unacceptable and can claim lives in emergencies. At the beginning of 2021, plans to reform the central on-call system were launched, including the fact that the systems maintained in parallel were unnecessary (ambulance, GP, emergency care) and that conflicts between the municipalities forced into the alliance caused most of the problems. In the opinion of the decision-makers, therefore, this is an organizational inadequacy and not a lack of financial resources.
The basis of continuously available health care is the general practitioner and the pediatrician, who, together with the medical on-call services, must provide the needs and requirements of the residents of the practice 24 hours a day. The territorial care system includes the care obligation of the resident of the area. When organizing care, it must be taken to ensure that care is available at well-planned times. The walls of the GP system have been collapsing for a long time, and the most obvious evidence of this has been the inadequate functioning of the central on-call system. In the case of on-call care, every minute counts, it is important that the patient has access to life-saving and prevention of serious or permanent damage to health as soon as possible.[1] One consequence of the increasing workload on primary care is increased waiting times, which, however, are most unacceptable and can claim lives in emergencies. At the beginning of 2021, plans to reform the central on-call system were launched, including the fact that the systems maintained in parallel were unnecessary (ambulance, GP, emergency care) and that conflicts between the municipalities forced into the alliance caused most of the problems. In the opinion of the decision-makers, therefore, this is an organizational inadequacy and not a lack of financial resources.
The current structure is unsustainable and this is mostly due to organizational inadequacies, however, the solution chosen is, in our view, not only appropriate to the roots of the problem, but also to symptomatic treatment.
Figure 1. Number of GP surgeries nationwide
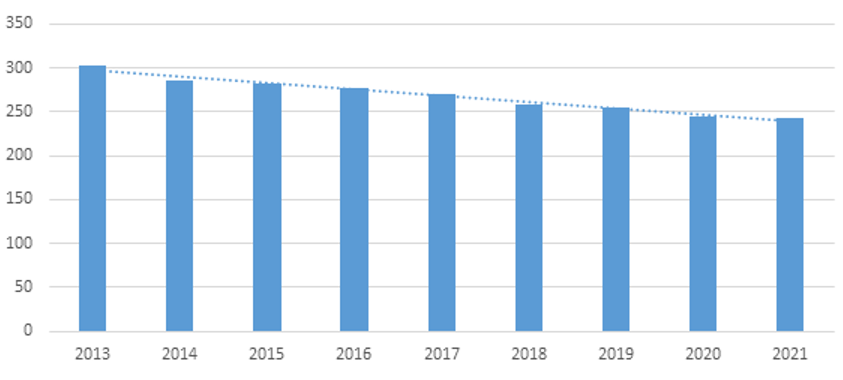
Source: NEAK[2]
After all, the biggest fault of the on-call system was the loss of efficiency in cases of the increasing workload of already overburdened GPs, often retired, while the burden on a care system (ambulance service) with a similar problem was without adequate financial and human resources and consistent organizational solutions.
1. Veterinary horse of the reforms: On-call duty
The National Ambulance Service is a central budgetary body under the authority of the Minister for Health, which divides the country into seven regional centers. OMSZ’s participation in on-call care is not new. According to the Government Decree of 2004, in the framework of primary care, the out-of-order performance of general practitioner duties must be performed through an on-call service or a central emergency service, in which case the general practitioner cooperates with the ambulance service. [3] Currently, the central medical on-call system is part of the primary care of the general practitioner, which helps to perform the “gatekeeper” function of this layer by taking a significant burden off the shoulders of the inpatient care system. According to the plans, following the successful pilot project in Hajdú-Bihar County, the on-call services would have ceased to exist by 2022, and district centers under the auspices of the OMSZ would have been established.
The importance of the reorganization is rooted in the fact that the lack of human resources in primary care is also felt during the provision of services. Most GPs retire, so there are age-related drop-outs and workloads. In addition, pediatricians are more affected, as they cannot be replaced by other doctors due to legal constraints, so their activities can be concentrated in fewer places.
Figure 2. Number of GP patients between 2010-2019
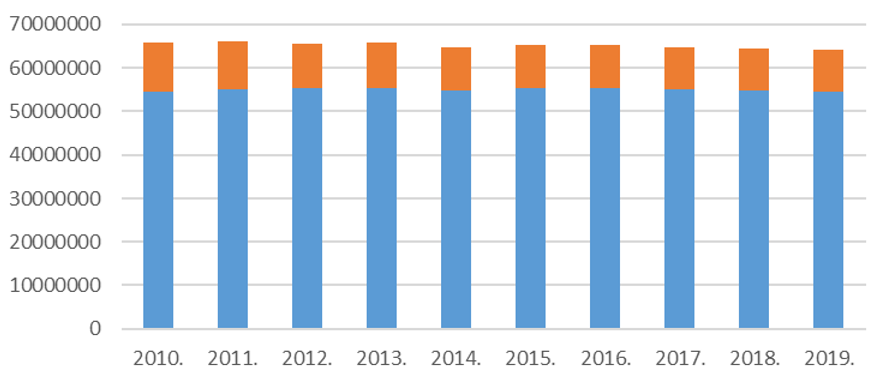
Source: NEAK
The aim of the change is to reduce the number of on-call sites (by establishing district centers), in the coordination and efficient operation of which the OMSZ would play a dominant role. The basic idea is not from the devil, and the involvement of the ambulance service in organizational matters in this way could be positive, but due to low salaries, lack of infrastructure, and lack of professional esteem, this organization also has difficulty in performing its tasks. This is also shown by the fact that from 2022 the central watch system was not operated by the OMSZ.
2. Funding issues
The services are financed from the Health Insurance Fund, as are other areas of health care. The basic amount of remuneration is HUF 42 per person, which varies by the multiplier specified by law. [4]
In settlements with a population of up to 40,000, out-of-hours general medical care can be provided through a central duty, in which case the health care provider is entitled to an increased fee (especially in addition to the provision of a dispatcher service). However, despite the increase in GP salaries in 2021, the central emergency department will not be able to compete with the outsourced hourly rates for emergency care wards as well as inpatient wards.
Thus, the mandatory fulfillment of adequate general medical care required by local governments in the Act on the Local Governments of Hungary[5] also imposes a significant burden on local entities, as they are often forced to balance it due to low funding. However, the quality of GP care depends on the economic strength of the municipality.
While according to NEAK data, there are 665 vacant GP practices in March 2022, this number is “only” 645 in June 2021, of which 24 have been vacant for nearly 15 years, 60 for more than 10 years, and 160 for more than 5 years. It appears that the 70% increase in the level of primary care wages since 2010 is not enough to deal with vacant practices, which is a problem in on-call care, among other things. The government’s solution, in addition to placing central services in the OMSZ, is to support the encouragement of communities of practice to address not only primary care problems but also to transfer some of the outpatient care to this scheme.
In our view, however, enforcing this form of cooperation also raises dilemmas. The rate of the increase in the salary of a general practitioner was made dependent by the legislator on the rate of cooperation (close 100%, loose 80%, no 30%). With the narrowing of the range of opportunities, the profession, which is already struggling with a lack of human resources, has received another blow. As a general rule, European Union law provides for a general prohibition of State aid, as provided for in Article 107 (1) TFEU.[6] Only subsidies which come from State resources in such a way that they confer an economic advantage on those concerned and are not granted in a general manner (selective) and that the aid affects or is likely to affect competition and trade between the Member States are prohibited. However, primary health care falls within the category of services of general interest, which is not covered by the EU framework (nor Article 107 TFEU) but must be governed by the provisions of the Member States, so that the solution adopted by the legislator does not constitute a prohibited subsidy. [7]
3. Hajdú-Bihar County: Sample project
There are eighty-one municipalities in Hajdú-Bihar County and the area had twenty-one duty centers. In the pilot project launched in the summer of 2021, ten district centers under the control of the OMSZ would have been established instead of the latter, which will be operated from Debrecen and Hajdúszoboszló. It is planned that from January 2022, this structure would have prevailed throughout the country, however, the problems and difficulties that arose did not allow it.
In our opinion, the transformation is necessary and under the direction of the OMSZ, not only cost reductions would be achieved, but the reorganization would provide patient care and emergency care. The reason for this is that the current form of the GP system is unsustainable, due to the lack of human resources and the professional staff working as retirees.
4. Rescue officers
The new system is based on ambulance officers (health professionals with higher education). Involving them in on-call care strengthens effective patient care, as they can perform most medical interventions, but they are also rooted in their greatest limitations, as they do not include needs that are as common as prescribing or a funeral visit.
Another problem is that the new system has been set up so quickly that it is difficult to carry out the increased tasks while increasing the shortage of human resources.
In our view, more experienced rescue officers would be needed and some of the legal restrictions could be reconsidered in order to effectively ensure adequate patient care.
5. Organization and information
In Hajdú-Bihar county, two companies performed on-call tasks: az Országos Orvosi Ügyeleti Kft. és a Debreceni Alapellátási és Egészségfejlesztési Intézet.
These organizations employed GPs who were on call in the county. After the OMSZ took over, the channeling of the former GPs into the new system was (and still is) extremely slow, which also made it difficult to implement an effective on-call system. The effectiveness of the reorganization, which began barely half a year ago, is further weakened by the fact that patients have difficulty adapting to changed circumstances. For example, an old phone number that is no longer in use is often called.
6. IT development
In order to minimize costs and perform tasks efficiently, a modern IT infrastructure is required, which ensures a proper connection between the OMSZ and the general practitioners and patients.
As the on-call service is used in an emergency, there would be a need for quick and easy IT services and support for the work of the OMSZ. The current system is outdated, unsuitable for responding to the challenges of the age, so an IT investment that is currently costly but profitable in the long run would be good.
7. Financing
As a result of the Health Service Legal Relations Act,[8] the salaries of GPs have increased significantly. The consequence of wage increases is that fewer and fewer doctors are on duty (in addition to performing their basic duties). In contrast, the wages of nurses have not changed, so those with experience often look for a more lucrative job, which makes it difficult for young people to transfer knowledge easily and quickly.
Summary
The reorganization of the on-call system is important as there is a shortage of human resources in primary care. Most GPs are retired, so they are expected to be out of work and less burdened by work.
In our opinion, the organization of the on-call system under the control of the OMSZ would be suitable for solving some of the current problems affecting primary health care, however, the existing legal constraints and the inconsistency of implementation lead to systemic problems. This, in turn, delays changes to the on-call system at the national level. In our opinion, it would be worth considering extending the powers of ambulance officers, raising the salaries of OMSZ employees, and implementing modern IT solutions to reduce the burden on the general practitioner system, which is struggling with a lack of human resources and thus improve the efficiency of on-call care.
Authors: Máté Sándor Deák, Assistant Lecturer at the Faculty of Public Health of the University of Debrecen, and Dr. Dóra Lovas, Assistant Lecturer at the Faculty of Law of the University of Debrecen; Research fellow at MTA–DE Public Service Research Group
The study was made under the scope of the EFOP-3.6.1.-16-2016-00022 “Debrecen Venture Catapult Program”.
For a list of references, click HERE.
[1] Article XX. The Fundamental Law of Hungary (25 April 2011).
[2]http://www.neak.gov.hu/felso_menu/szakmai_oldalak/publikus_forgalmi_adatok/gyogyito_megelozo_forgalmi_adat/fin_adatok_szolgaltatonkent.html [accessed March 2, 2022]
[3] 47/2004. (V.11.) ESzCsM decree on certain organizational issues related to the continuous operation of health care
[4] Article 19. 43/1999. (III.3.) Government Decree on the detailed rules for issuing health services from the Health Insurance Fund
[5] Article 13. 4. Act CLXXXIX of 2011 on Local Governments of Hungary.
[6] Article 107. (1) Treaty on the Functioning of the European Union, OJ C 326, 26.10.2012, pp. 0001– 0390 (’TFEU’)
[7] Article 14. and 106. TFEU, and Article 26. Treaty of Lisbon amending the Treaty on European Union and the Treaty establishing the European Community, signed at Lisbon, OJ C 306, 17.12.2007, pp. 1–271.
[8] Act C of 2020 on Health Service Legal Relations.
